When Christopher Johnson started feeling a little under the weather, he didn’t immediately think COVID-19 – after all, he was fully vaccinated.
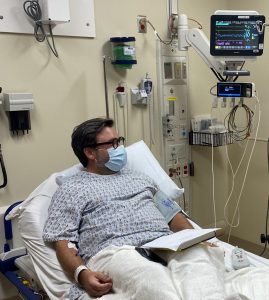
Christopher Johnson receives sotrovimab, a COVID-19 outpatient treatment, at UPMC Passavant Cranberry.
But when his symptoms – a terrible cough, shortness of breath, fever – rapidly became more severe than a typical cold, he got tested and, sure enough, came back positive for COVID-19. The co-CEO of TeleTracking, which specializes in health system technology, immediately sought out the best option for care.
“I knew about monoclonal antibodies through the work that TeleTracking has done with the U.S. Department of Health & Human Services, so I called up my primary care physician and said, ‘I want this treatment,’” said Johnson, 49, of Sewickley. “He quickly got me referred and scheduled at UPMC Passavant in Cranberry.”
And when Johnson went in for his outpatient infusion with the one-time treatment shown to significantly reduce the risk of an outpatient needing to be hospitalized for COVID-19, he received a pleasant surprise: He’s the first reported in the U.S. to receive sotrovimab, a monoclonal antibody created by GSK and Vir Biotechnology, under the recent FDA emergency use authorization.
His infusion was followed the next day by UPMC’s second patient to receive sotrovimab: Kristin DeLuca, 51, of Whitehall.
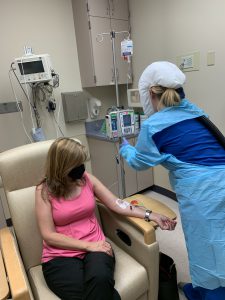
Kristin DeLuca receives receives sotrovimab, a COVID-19 outpatient treatment, at UPMC South Side.
DeLuca also contracted COVID-19 while fully vaccinated. Even though her symptoms were relatively mild, her pulmonologist encouraged her to receive monoclonal antibodies because she has a severe form of asthma and referred her to UPMC South Side.
“It was easy, perfectly painless,” said DeLuca, director of operations at the Omni William Penn. “I would 1,000% encourage anyone who thinks they might have COVID-19, whether they’re vaccinated or not, to get tested and get monoclonal antibodies if you’re eligible.”
Dr. Graham Snyder, medical director of infection prevention and hospital epidemiology at UPMC, said it isn’t surprising that some fully vaccinated people get COVID-19. While the three COVID-19 vaccines available in the U.S. are all very effective, none are an absolute guarantee against contracting the virus.
“What we are seeing – and what seems to have happened with these two patients – are some breakthrough infections,” said Snyder. “That doesn’t mean the vaccines don’t work. In fact, they work very well to keep you from severe disease. But that doesn’t mean COVID-19 can’t be serious, or rarely fatal, in people who have gotten a vaccine. It’s important to get tested if you think you might have COVID-19 and, if you’re positive, talk to your provider about monoclonal antibody treatment.”
Both Johnson and DeLuca have been enrolled in UPMC’s OPTIMISE-C19 study, which randomizes patients to the monoclonal antibody treatments available in the U.S. – currently sotrovimab or Regeneron’s combination of two monoclonal antibodies. Both are typically given through a one-time intravenous infusion that takes less than hour.
Through the OPTIMISE-C19 study, UPMC is comparing available monoclonal antibodies with the goal of learning which works best in which patients and against which variants. The study is being conducted through UPMC’s innovative “learning while doing” method of providing the best possible available care, while collecting and analyzing data to make that care even better for future patients. The health system expects to share early data in the coming month.
Johnson and DeLuca are both in good health less than a week after their monoclonal antibody infusions.
To learn more about monoclonal antibodies and treatment eligibility, visit www.upmc.com/antibodytreatment or call 866-804-5251.