As public health authorities raise concerns about a tuberculosis (TB) resurgence fueled by the war in Ukraine and COVID-19-related disruptions in preventive care, new research is identifying which aspects of the immune response determine whether the body can keep TB infections under control.
The findings, made by a team of investigators at the University of Pittsburgh, Massachusetts General Hospital, Massachusetts Institute of Technology and Harvard University and published in Immunity, point to potential strategies for the development of new vaccines and therapeutics.

Dr. JoAnne Flynn
More than 1.7 billion people—or a quarter of the world’s population—are infected with Mycobacterium tuberculosis, the bacterial strain that causes TB. For years, scientists have been working to develop an effective vaccine, but current TB vaccines are only partially protective.
Although the body’s immune system can often keep M. tuberculosis infections under control, resulting in asymptomatic infections, approximately 1.5 million people die from TB yearly. According to infectious disease experts, the war in Ukraine might drive this number even higher as people huddle in bomb shelters with limited access to clean water and sanitation. The COVID-19 pandemic has also slowed TB control efforts due to reduced access to medical care.
“TB is a horrible disease, primarily affecting people in developing countries. Treatment of TB is long and requires using multiple drugs, and drug-resistant infections are even more difficult to treat,” said co-senior author Dr. JoAnne Flynn, distinguished professor of microbiology and molecular genetics and a member of the Center for Vaccine Research at Pitt. “To truly make a difference in the TB epidemic, we need improved vaccines. But to guide vaccine development, we need a better understanding of the immune responses that help kill bacteria at the site of infection, as well as those immune responses associated with lack of control of infection.”
In response to M. tuberculosis infection, which usually occurs in the lungs, the body forms granulomas—tiny clusters of immune cells recruited to respond to the infection and other immune cells already present in the lung tissue. In some granulomas, immune activity promotes bacterial clearance, but in others, bacteria persist and grow. These different granuloma responses can even be seen in the same individual.
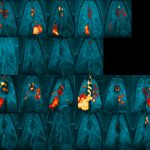
To identify which cellular and molecular features control whether a granuloma would resolve on its own or persist for a long time, scientists in Dr. Flynn’s lab developed a monkey model that recapitulates the features of human TB. They also devised ways to track and quantify bacterial burden in individual granulomas.
In collaboration with biomedical engineers and immunologists at the other institutes, the Pitt team revealed that bacterial persistence occurs in granulomas enriched with cells and functions that are generally associated with wound healing, suggesting that the lung is trying to wall off the infection. In contrast, granulomas that supported bacterial clearance are characterized by T cells that produce factors such as cytokines and cytotoxic molecules that can interact with infected cells and kill the bacteria.
“Our findings highlight new targets—such as specific cell subsets—to guide next-generation vaccines,” said co-senior author Dr. Alex Shalek, associate professor of chemistry at MIT. “We can also begin to consider how we might directly manipulate entire granulomas through modulating intercellular signaling to combat the bug more effectively.”
Until the COVID-19 pandemic, TB was the leading cause of death from infectious diseases worldwide, emphasized co-senior author Dr. Sarah Fortune, professor of immunology and infectious diseases at Harvard University. Unlike COVID-19, which is caused by a virus, TB is caused by bacteria, and current treatment involves multiple months of aggressive antibiotic therapy.
“This study’s new insights into how the immune system clears, or in some cases helps, TB are critical in figuring out what a new vaccine should do,” says Fortune.