A patient in the Williamsport, Pennsylvania, area needs a liver transplant. Up until about a year ago, the only option was to wait for a deceased donor’s liver — along with close to 14,000 other patients on the national liver transplant list.
But the national liver transplant waiting list is just the beginning of a very complicated process for someone in need of a liver transplant.
To be added to the waiting list, the patient must be evaluated using the Model for End-Stage Liver Disease (MELD), which results in a score. MELD scores determine how desperately the patient needs a liver transplant; the higher the score, the more urgent the need.
MELD scores are re-evaluated from time to time, but they aren’t the only predictors for wait time on the transplant list. Other predicting factors include supply and demand for livers in the region, geographic proximity to the donated liver, blood type, body size, and the donor’s age.
Once the patient is added to the waiting list, they may wait up to two years to receive a liver from a deceased donor. During the wait, their disease may progress, and their overall health may become too poor to receive a new liver.
UPMC Susquehanna saw an opportunity to help patients in their community facing the long list and long wait. They wanted to give their patients access to UPMC’s living donor program by opening a liver transplant evaluation clinic.
Living-donor liver transplants take part of the healthy liver of a living person and use it to replace the unhealthy liver of another person. This type of transplant gives patients an option with life-saving advantages — shorter wait times, improved long-term outcomes, increased treatment options, and quicker recovery times. The procedure also increases the number of available deceased organs for patients in desperate need.
The first and only clinic of its kind in the Williamsport area, the UPMC Liver Transplant Evaluation Clinic at UPMC Susquehanna officially opened in May 2018.
“Since the moment we opened the clinic, our patients have been banging down our doors to be evaluated,” said Shannon Gottschall, practice manager, Digestive Disease Center, UPMC Susquehanna.
The Perfect Addition
The clinic has been a perfect fit and addition to the Digestive Disease Center. Gottschall’s team, which is made up of Dr. Puneet Basi, hepatologist and gastroenterologist, and five certified physician assistants, Megan Colvin, Ashley Imrisek, Isabella Malinowski, Helen Miller, and Ashley Roman, regularly sees patients facing liver disease. As patients are being seen, the physician assistants are keeping LDLT in mind.
When a patient gets to the point where they meet the requirements for living-donor liver transplant, the physician assistant reviews their case with Basi, and together they decide if that patient should be referred for evaluation at the clinic.

Thanks to the initial groundwork done at UPMC Susquehanna, when Dr. Swaytha Ganesh, medical director for UPMC’s Living Donor Program at the Thomas E. Starzl Transplantation Institute, visits the clinic, she can hit the ground running.
Ganesh travels with her team from Pittsburgh to Williamsport every other month to make final evaluations on the patients who have agreed to be seen at the clinic. Her team’s services include imaging scans, blood tests, radiology, diagnostic testing, consults, exams, and continuing education.
“Having a hepatologist on-site puts us in a unique situation,” said Gottschall. “Because Dr. Basi reviews the patients and refers them to the clinic, by the time Dr. Ganesh sees them, she’s pretty certain she’ll be able to get those patients approved for living-donor transplants.”
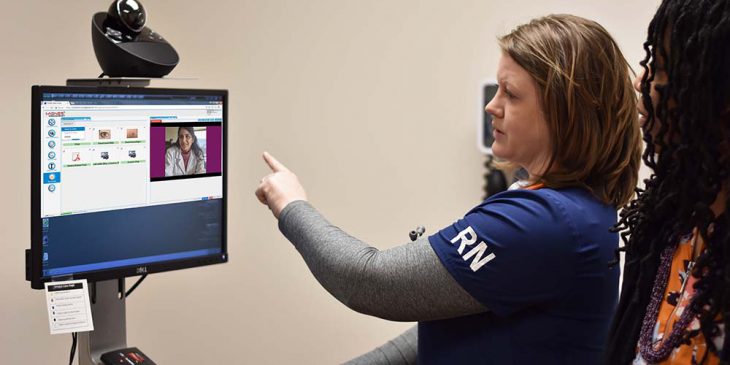
After a patient has been approved for living-donor liver transplant and is finally ready for pre-operation evaluation, UPMC Susquehanna has eight rooms waiting for their arrival and set up with telemedicine capabilities.
“Instead of the patient taking time off work, having somebody drive with them to Pittsburgh, paying for a hotel room, and setting up a bunch of different appointments with their doctors — and this is all hoping they are healthy enough to make the trip,” said Gottschall. “They can stay here with us for a four-to-five hour visit, where they will speak face to face with each of their doctors via telemedicine.”
This is one of the biggest benefits to patients — they are already familiar and comfortable with the staff at UPMC Susquehanna, and they don’t have to fear traveling to and from Pittsburgh multiple times just to have access to the Living Donor Program.
Right now, there are approximately 27 patients at UPMC Susquehanna waiting to be evaluated by Ganesh, and her goal is to introduce every single one of those patients to the concept of living-donor transplant.
Extending Knowledge and Access
There are around 14,000 people on the national liver transplant waiting list, and approximately 8,250 liver transplants took place in 2018. Of those, only about 400 were living-donor liver transplants.
This is one of the major reasons why living-donor liver transplant is a priority for UPMC, and why UPMC has opened several liver transplant evaluation clinics throughout Pennsylvania. UPMC Hamot opened their clinic in Erie in February 2017, and UPMC Pinnacle opened their clinic in Harrisburg in June 2018. Both of these clinics provide evaluation services and education to area patients who have never had access to living-donor liver transplants in the past.
Ganesh and her team spend time at each clinic helping patients — and potential living donors — understand all the reasons this option is a viable alternative to the waiting list.
 Because the liver regenerates, the living donor (who can be a relative, friend or even a stranger) can donate a portion of his or her liver to the patient. It typically only takes about eight to 10 weeks for the liver to grow back to full size. For the patient, finding a suitable living donor allows them to bypass the national liver transplant waiting list and receive their transplant before becoming critically ill.
Because the liver regenerates, the living donor (who can be a relative, friend or even a stranger) can donate a portion of his or her liver to the patient. It typically only takes about eight to 10 weeks for the liver to grow back to full size. For the patient, finding a suitable living donor allows them to bypass the national liver transplant waiting list and receive their transplant before becoming critically ill.
And, when the patient receives an organ from a living donor, he or she typically has better results because the donor is a better genetic match, the treatment options are increased, and the recovery times are quicker.
“UPMC believes no one should die waiting for a liver transplant,” Ganesh said. “Living-donor liver transplant is possible for virtually every person on the waiting list. As pioneers in the field of liver transplant, UPMC is on a mission to make everyone aware of the life-saving procedure, one which we offer as first-line option rather than a last resort.”
To learn more about the Living Donor Program, visit www.lifechangingliver.com.