Autoimmune disorders of the skin depend on circulating T cells, but a common weakness could point to a cure
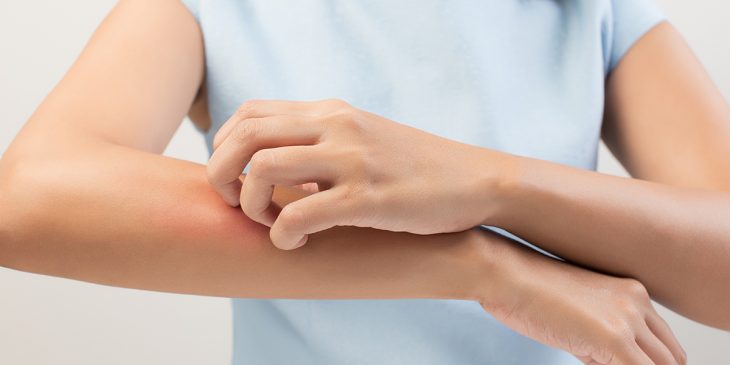
Psoriasis, alopecia, eczema and even cutaneous lymphoma can all be traced to an immune response run amok – with rogue memory T cells setting their sights on native skin cells rather than invading pathogens.
In an article published today in the journal Immunity, University of Pittsburgh researchers found a chink in the armor of these marauding cells that could lead to therapies to knock out autoimmune responses in the skin and keep them from recurring.
“Previously, we discovered these memory cells that live in the skin depend on this cytokine, TGFβ, and that’s great because that means you have a pathway, a circuit to interrupt, to treat these diseases,” said senior author Dr. Daniel Kaplan, professor of dermatology and immunology at Pitt. “The problem is that there are also circulating memory T cells throughout the body, so you can chase the resident memory cells out of the skin, but they’ll just come right back.”
 To show how important these circulating, skin-homing memory T cells are, Kaplan’s team, led by postdoctoral researcher Dr. Toshiro Hirai, infected mice with vaccinia virus, harvested the newly imprinted circulating T cells and then transferred them into a new crop of mice, some of which were genetically engineered to lack functional TGFβ in the skin.
To show how important these circulating, skin-homing memory T cells are, Kaplan’s team, led by postdoctoral researcher Dr. Toshiro Hirai, infected mice with vaccinia virus, harvested the newly imprinted circulating T cells and then transferred them into a new crop of mice, some of which were genetically engineered to lack functional TGFβ in the skin.
If these circulating T cells depend on TGFβ, and immune responses in the skin in turn depend on these cells, Kaplan reasoned, the functional benefit of the transplanted cells should be lost in the mutant mice. That’s exactly what his team found.
The recipients with normal immune systems were effectively vaccinated against the virus – meaning their skin was relatively virus-free after the animals’ first encounter with the bug – while the mutant mice without TGFβ in the skin were not so lucky. Without the memory T cells, they were not able to mount a defense against the virus.
In this example, the circulating cells were beneficial for warding off skin infection, but when the immune system turns against the body during autoimmune diseases of the skin – like alopecia, eczema and psoriasis – the same cells could play a detrimental role.
Kaplan and colleagues were surprised to discover not only that these circulating cells go to the skin, but that they also depend on TGFβ, just like the T cells that set up shop there.
“That they go to skin is new and that they depend on the same factor is also new and exciting,” Kaplan said. “That means if you inhibit the pathway you can get rid of both.”
He envisions a topical cream loaded with small molecule TGFβ inhibitors that would defend the skin under siege, while leaving the rest of the immune system intact. Testing in mice is already underway.