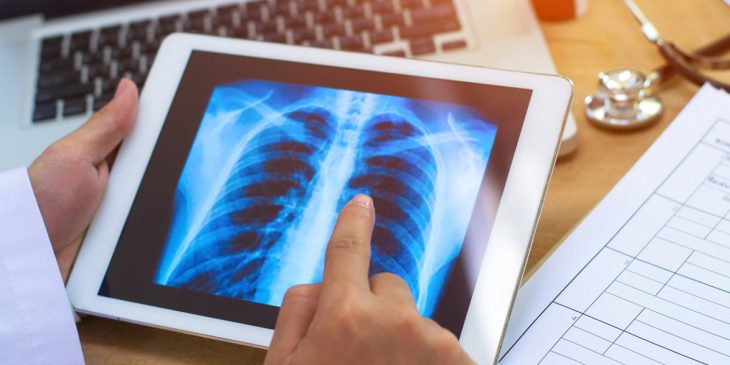
The UPMC Lung Transplant Program has performed more than 2,000 lung transplants, the most of any center in the country according to the United Network for Organ Sharing Data. For patients, sometimes the most grueling part of the process is waiting months — and in some cases, years — for a set of lungs to become available to them through an organ donor. There are currently 1,500 people in need of a lung transplant in the U.S.
During the transplant process, while patients are anxiously waiting for a call, the team of transplant specialists at UPMC are busy trying to track down the best possible sets of lungs for them. Sometimes during an evaluation, something called a “dry run” can occur. While this may seem like a setback for the patient, it’s actually a valuable part of the transplant process. To learn more, we asked Dr. Jonathan D’Cunha, chief of lung transplantation at UPMC, to help explain what dry runs are, why they happen, and what transplant patients should expect if it ever happens to them.
What is a dry run?
When a patient gets listed for a lung transplant, he or she is waiting for lungs from a donor to become available. The process truly begins when a seemingly healthy pair of lungs come in from a deceased organ donor. If the lungs turn up in a remote hospital, which can sometimes be hundreds of miles away, we send out a team to assess and evaluate them in person so we can determine if the lungs are a good fit for our transplant patient who needs them. All the while, we are contacting the patient to let him or her know that a set of lungs has been found and asking them to come in and prepare for surgery.
Sometimes, the lungs assessed by our remote team aren’t a good fit, and by that point, the patient is most likely already at the hospital. That’s when we have to inform the patient that the lungs weren’t a perfect match and the surgery won’t happen– AKA, a dry run has taken place. It’s a disappointing but extremely important step in the transplant process.
Why do dry runs occur?
- The sicker a patient is and the higher his or her Lung Allocation Score, the more susceptible they are to dry runs. If you think about it, the lungs are different than any other organ – they are exposed to the environment. We have to evaluate lung function, quality and size, and we have to make sure the lungs don’t have pneumonia or infarctions (blood supply loss).
How often do dry runs occur?
- Dry runs occur about 10 to 20 percent of the time. At a high-volume center like UPMC, we have the luxury of being able to go out and look at lungs aggressively. I always tell patients that’s a good sign because it proves that we care about our patients and the surgery outcome.
What typically happens from a clinical point of view when a dry run takes place? How do you tell the patient?
- Transplant patients come in months before they are placed on the transplant list. During that time, we host an educational program where we teach them about the lung transplantation process. We set their expectations early for a possible dry run so they know what they’re up against. When they get called in for a transplant, they get excited, so we always talk to them and make sure they know that a dry run could be a possibility. By setting expectations ahead of time, the usual response when we tell them it’s a no-go is a positive one: ‘Thank you for being so careful with this.’
Is there anything else that patients and their families should know about dry runs?
- I try to use analogies for patients to understand dry runs. Think about them in terms of wanting to purchase a house and looking up pictures online. The pictures and logistics of the house might look great from your computer screen, but then you do an actual walk-through and it’s not what you thought. You might have to look through several “houses” before you find the right one.
At UPMC, we make sure that patients are getting the best lungs available to them. In 2018, a new medical innovation known as Ex Vivo Lung Perfusion (EVLP) is allowing us to take lungs we aren’t sure about and actually put them to the test. This allows our evaluations to be much more efficient and accurate. Also, with the new lung allocation system that went into place at the end of 2017, we are doing more remote evaluations, especially for sicker patients. With this new system in place, there is a potential for us to have more dry runs, but again, that’s not a bad thing. It just means we are coming across lungs at such a rate that we are able to be selective, and that is the best-case scenario for our patients.
To learn more about the lung transplant program at UPMC, visit www.upmc.com/services/transplant/lung.