After an exhaustive look back at 10 years of laboratory samples, UPMC infectious disease experts are confident that the hospital system hasn’t experienced the latest “superbug” to alarm federal public health officials.
But, that doesn’t mean UPMC is lowering its guard against Candida auris, a stubborn pathogen first reported in the U.S. in November.
“We’ve had several conferences with our infectious diseases physicians, infection control practitioners and clinical microbiology laboratory staff to prepare for C. auris,” said Dr. Minh-Hong Nguyen, director of UPMC’s Antimicrobial Management Program and Transplant Infectious Diseases. “We have mechanisms in place to diagnose infections immediately, and we have plans in place to prevent its spread in the hospital.
“We’ve also consulted with the U.S. Centers for Disease Control and Prevention and obtained reference samples. Along with Dr. William Pasculle, director of UPMC’s clinical microbiology laboratory, we are fully confident that we have all the proper testing equipment to detect C. auris in real time.”
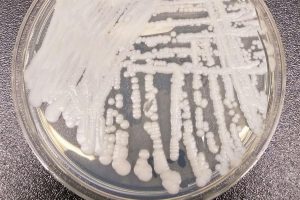
C. auris causes bloodstream and other infections that are resistant to most antifungal drugs (often referred to as “superbugs”). These infections have been associated with mortality rates of up to 50 percent among patients hospitalized at other centers. C. auris is typically recovered from patients who are already hospitalized for a different reason. It was first identified in 2009 in Japan, and has since been found in more than a dozen countries.
Nguyen and her colleague Dr. Cornelius J. Clancy, director of the Pitt Division of Infectious Diseases’ Mycology Program, work in a lab connected to UPMC Presbyterian and Montefiore hospitals. They note that, as an academic medical center, UPMC has sophisticated equipment outfitted with lasers that can deliver just the right amount of energy to permit diagnosis of C. auris without obliterating it. Pulsed lasers separate the pathogen so scientists can then determine its biomolecular signature and identify it.
Being able to rapidly and accurately diagnose C. auris means that clinicians can quickly move an infected patient into an isolation room, provide medications and care to help fight the infection, and create the best possible odds to avoid spreading it to other patients.
“Clinically, the course of C. auris infections isn’t much different than other Candida species that more commonly infect hospitalized patients,” Clancy said. “However, it has proven incredibly difficult to eradicate once it enters a hospital, causing long-standing outbreaks. This is why early detection measures, like what we have put in place at UPMC, are so important.”
Clancy and Nguyen said public health officials still don’t know whether C. auris will be widespread – much like Carbapenem-resistant Enterobacteriaceae, which emerged and spread across the U.S. several years ago – or be contained to single hospitals in case-by-case outbreaks. The CDC has reported cases and outbreaks in New York, Illinois, Maryland, Massachusetts and New Jersey.