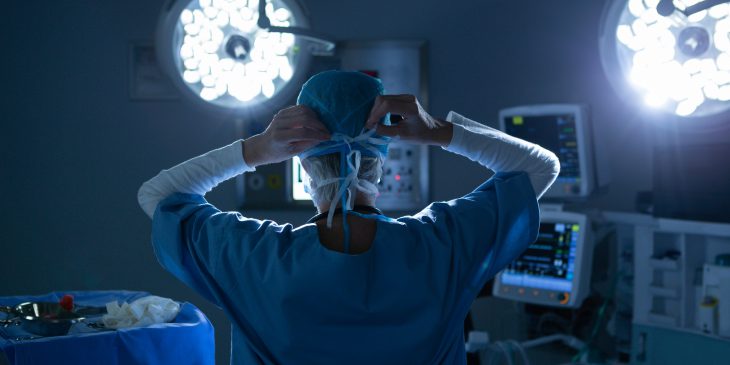
Sara Myers, M.D., Ph.D.
Surgery is well-documented as a male-dominated field – less than 10% of full professors in academic surgery departments in the U.S. and Canada are women. Now a University of Pittsburgh School of Medicine-led study published today in JAMA Surgery shows the issue isn’t surgical ability.
It may be the more insidious influence of gender stereotypes during training that boosts male surgical trainees’ confidence, while dampening that of their female counterparts.
In the two-phase study, lead author Sara Myers, M.D., Ph.D., general surgical resident in Pitt’s School of Medicine, and her colleagues recruited 86 general surgery residents from three academic medical centers. First, they assessed the association between perceived gender bias and career engagement. It wasn’t the women’s engagement that was measurably affected by perceiving pro-male bias, it was the men’s – and they had higher career engagement when they had higher perception of pro-male bias in their environment.
In the second phase of the study, the research team gave the residents a surgical skills assessment test after exposing half the participants to pro-male bias in surgical skills and half to no bias. There was no appreciable overall difference in surgical skill performance between men and women.
But when Myers and her colleagues drilled down and assessed the participants’ susceptibility to “stereotype threat,” which is the risk of reinforcing a negative stereotype about a social group that someone identifies with, they found that women who were more susceptible performed worse on the surgical skills test.
“It is important to note that there was no difference in skill between men and women. It was only after factoring in sensitivity to the negative stereotype that we were able to appreciate performance differences by gender,” Myers said. “This is, perhaps, because not all individuals are vulnerable to negative stereotypes or bias. Some women hear negative stereotypes and have the opposite response: ‘I’ll show them!’ and end up performing much better than men.”
The researchers postulate that more subtle findings like this could lead to less engagement, cascading into reduced academic performance, burnout and attrition among women in academic medicine.
“When a stigmatized individual has his or her executive functioning siphoned away from the task at hand [such as when worrying about gender bias], they perform worse,” Myers said. “We need to nurture everyone to be the best they can be.”
Myers believes that proven strategies to reduce stereotype threat in other fields could translate into surgical training, including increasing visibility of minority groups, removing gender bias cues and reinforcing similarities in interests among residents, rather than focusing on differences.
“If a singular, subtle and transient exposure to a stereotype could negatively impact surgical skill performance, could this possibly translate to harm in a patient?” Myers asked. “This possibility, while not addressed in our investigation, should compel us as a community to take actions that change the prevalence of these stereotypes and associated bias in our culture.”